- 25/02/2026
- Dr. Raviram
- 0 Comments
- Piles
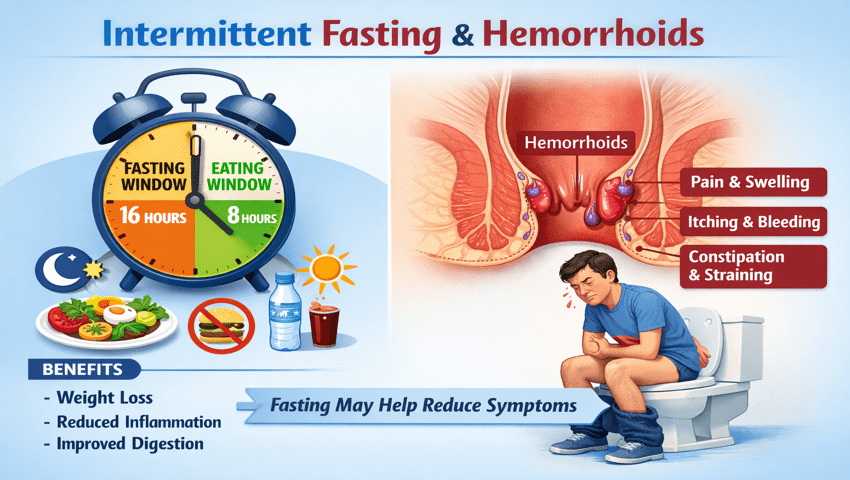
Intermittent Fasting and Hemorrhoids: What You Should Know
Intermittent fasting (IF) has become a massive global trend for weight loss, improved metabolism, and gut resting. But if you suffer from swollen rectal veins, you might be wondering about the connection between intermittent fasting and hemorrhoids.
Patients frequently ask Dr. Raviram S., a leading Piles Specialist in Thrissur: “Does fasting help hemorrhoids, or does it make them worse?” The truth is, fasting and piles have a complex relationship. While losing weight can reduce pressure on your pelvic floor, poor fasting habits can lead to severe constipation—the number one trigger for hemorrhoid flare-ups. In this article, you will learn how intermittent fasting affects bowel movements, whether it is safe for piles patients, and how to fast wisely without irritating your condition.
Does Intermittent Fasting Help Hemorrhoids?
If you are searching for whether fasting for hemorrhoids is a good idea, here is the quick, medically backed answer:
- It may help if constipation improves: Giving your digestive system a break can reduce bloating and gut inflammation.
- It may worsen piles if dehydration occurs: Not drinking enough water during fasting windows leads to hard, dry stools.
- It is not a permanent cure: Does fasting cure hemorrhoids? Fasting cannot shrink existing enlarged, prolapsed veins.
- It depends on diet quality during the eating window: Breaking a fast with junk food will trigger immediate flare-ups.
If your piles are bleeding or causing severe pain, fasting alone won’t fix it. You need an expert diagnosis at a Proctology Clinic in Kerala at Thrissur Piles Clinic.
How Intermittent Fasting Affects Digestion and Bowel Movements?
- Changes in Stool Frequency During Fasting: When you restrict your eating window (like the 16:8 method), you consume fewer meals. Reduced meal frequency naturally means less waste is produced, leading to less frequent bowel movements. Because your gut rests, you might experience a slower gut movement (decreased peristalsis).
- Fasting and Constipation – The Hidden Risk: Many people ask, “Does fasting help constipation?” Usually, the opposite is true. When you eat less, your low fiber intake drops. Without enough bulk, stool sits in the colon longer, drying out. This leads to hard stools after long fasting hours, which require you to push harder in the bathroom—a direct cause of hemorrhoids.
- Role of Hydration in Preventing Piles Flare-Ups: Some people attempt water fasting to heal hemorrhoids. While water is crucial, prolonged water-only fasting lacks fiber. However, normal intermittent fasting requires excellent hydration. Your water intake importance cannot be overstated; maintaining an electrolyte balance ensures your stool remains soft and easy to pass.
Can Intermittent Fasting Reduce Hemorrhoid Symptoms?
So, is fasting good for hemorrhoids in any scenario? Yes, but indirectly.
- Reduced Inflammation and Weight Loss Benefits: Obesity is a major risk factor for piles because extra belly fat creates continuous lower abdominal pressure. By helping you lose weight, intermittent fasting relieves this pressure, reducing the daily strain on your rectal veins.
- When Symptoms Temporarily Improve: Some patients report that fasting and hemorrhoids interact well in the short term. Because they are eating less, they experience less bloating and improved digestion. Fewer bowel movements mean less friction on the anal area, giving an irritated, burning hemorrhoid a brief chance to calm down.
Can Intermittent Fasting Make Hemorrhoids Worse?
Yes, if done incorrectly. Will fasting help my hemorrhoids? Not if you make these common mistakes:
- Dehydration During Fasting: Forgetting to drink water during the fasting window causes the colon to absorb moisture from your stool, making it rock hard.
- Overeating During Eating Window: Binge eating large, heavy meals when your fast breaks overloads the digestive system, creating bulky stools that stretch the anal canal.
- Straining After Breaking the Fast: Hard stools require intense pushing. This straining inflames the blood vessels, leading to painful, swollen lumps.
- Increased Risk in People with Chronic Constipation:If you already struggle to go to the bathroom, restricting your eating schedule will likely make your constipation—and your piles—much worse.
Is Intermittent Fasting Safe for People with Bleeding Piles?
If you have actively bleeding piles, you must be extremely careful.
- When it may be unsafe: If your bleeding is causing weakness or anemia, fasting may lower your energy levels and blood sugar dangerously.
- Signs to stop fasting: Stop if you experience dizzy spells, severe constipation, or increased blood in the toilet bowl.
- When to consult a doctor: Do not rely on fasting to stop bleeding. Consult the Best Proctologist in Thrissur, Dr. Raviram S., immediately for a proper medical evaluation.
Best Diet Plan While Doing Intermittent Fasting with Hemorrhoids:
If you want to try IF while managing piles, what you eat during your opening window matters more than the fast itself.
High-Fiber Foods to Include:
To ensure fasting and piles don’t clash, break your fast with:
- Fruits: Papaya, apples (with skin), and berries.
- Vegetables & Whole Grains: Spinach, oats, brown rice, and lentils.
What to Avoid?
- Spicy food: Irritates the anal lining during a bowel movement.
- Processed food & Excess caffeine: These dehydrate the body and cause hard stools.
Ideal Hydration Strategy:
Drink 2–3 liters of water daily. Include hydrating fluids like coconut water or buttermilk during your eating window to keep your gut lubricated. (A temporary liquid diet for hemorrhoids can sometimes ease acute flare-ups, but should only be done under medical supervision).
Intermittent Fasting vs Regular Balanced Diet for Piles:
Which is better for long-term hemorrhoid relief? While IF is great for weight loss, a regular, high-fiber, balanced diet spaced evenly throughout the day is generally safer for piles. Consistent fiber intake keeps your digestive tract moving rhythmically, preventing the dry, hard stools associated with long fasting gaps. Why consistent fiber matters more than fasting: Soft, daily bowel movements are the ultimate defense against hemorrhoid pain.
When You Should Avoid Intermittent Fasting?
Do not attempt intermittent fasting if you have:
- Severe constipation that requires daily laxatives.
- Thrombosed hemorrhoids (a painful blood clot in the vein).
- Chronic bleeding leading to anemia.
- Just had surgery. If you recently underwent Laser Piles Surgery in Thrissur, your body needs consistent, nutritious, fiber-rich meals to heal properly.
Conclusion:
So, can fasting heal hemorrhoids? No. While weight loss from intermittent fasting can reduce pelvic pressure, the fast itself will not shrink or cure existing piles. In fact, if you don’t drink enough water, the resulting constipation will make your symptoms worse.
If diet and lifestyle changes aren’t giving you relief, it is time to seek professional help. You don’t have to live with the pain. At Thrissur Piles Clinic, Dr. Raviram S. offers the most advanced, Painless Piles Treatment in Thrissur. From expert dietary counseling to state-of-the-art Laser Piles Treatment in Thrissur, we provide comprehensive care tailored to your specific needs. Call now 9961001199 to connect with us!
